The outlook for the Covid-19 vaccine today can be partly seen from the tragic picture of the AIDS pandemic in the late 1990s and early 2000s, when pharmaceutical firms developed effective diagnostic and treatment tools that could save the lives of millions in poor countries, but were unwilling to share them.
 |
|
India begins a nationwide campaign for Covid-19 vaccination. |
The movement to enable access to AIDS drugs in countries like Brazil, South Africa, India, and Thailand through mandatory patent sharing with multinational corporation helped antiviral drugs reach accessible levels, falling in price from more than $10,000 per year to over $300, saving the lives of tens of millions of people and repelling the spread of AIDS.
Ethical conduct
The current global vaccine crisis comes from supply scarcity. Markets and patents are the fundamental reasons for restricting access to vaccines, and they are deeply rooted in the global intellectual property order, even when a public health crisis is at a serious level.
Last July, South Africa, and then India, submitted a proposal to the TRIPS (WTO Agreement on Trade-Related Aspects of Intellectual Property Rights) Council on intellectual property and public interest and a comprehensive and flexible approach to TRIPS to enable broad, flexible, and affordable access to vaccine patents and curative solutions in response to pandemics.
South Africa also mentioned the World Health Organization's (WHO) COVID-19 Technology Access Pool (C-TAP) initiative.
Since May 2020, C-TAP, launched by WHO in partnership with the Government of Costa Rica and 40 member state co-sponsors with the Solidarity Call to Action, has called to action the global community to voluntarily share knowledge, intellectual property and data necessary for COVID-19.
C-TAP is intended to provide a means to accelerate the development of products needed to fight COVID-19 as well as to speed up the scale-up of manufacturing and the removal of barriers to access, in order to make these products available globally.
However, this initiative has not been supported by multinational corporations.
The efforts of South Africa and India have not received necessary support from developed nations, even though they were backed by 140 other countries, and they were even stopped by developed countries, where national selfish vaccination programs have begun.
Many voices have called for ethical conduct raised in Western countries. Dr. Anthony Fauci, an infectious disease specialist for the US government, noted that the US can help strengthen global production capacity through policy interventions and require cooperation from pharmaceutical companies through loosening a number of patents, allowing the production of vaccines on a global scale wherever it is possible.
Western nations can promote global access to vaccines through patent sharing and support of vaccine producers.
Public-private partnership
 |
|
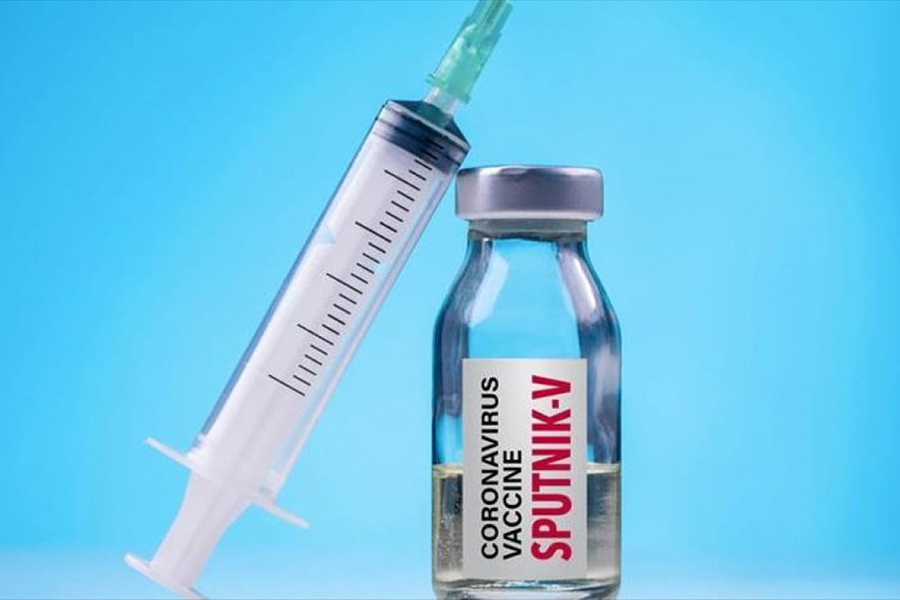
Russia has begun to supply Africa with its Sputnik V vaccine. |
First of all, vaccines come from public-private cooperation efforts as vaccine development is primarily funded by the public budget. The US and Europe have poured immense resources into vaccine research and development and vaccine pre-orders to eliminate risks for research firms.
The US spent $2.48 billion on a new vaccine at the National Institutes of Health (NIH)/Moderna, while the German government also provided $445 million to develop the Pfizer-BioNTech vaccine.
This engagement, along with the practice of forced licensing in treatment solutions, shows that the West can create pressure to force pharmaceutical companies to share inventions and technologies by providing first-time technology transfer and licensing fees through royalties per sales in low- and middle-income countries.
Politically, Western nations were warned by French President Macron at the G7 Summit held on Feb. 19 that Africa would switch to Russian and Chinese vaccines. This scenario threatens the influence and status of the West. The African Union announced it would receive 300 million doses of the Sputnik V vaccine from Russia in May. Expanding access to vaccines is a key element in strengthening the West's position in other countries.
Turkey signed an agreement to start production of Sputnik V, even though it has bought 50 million doses of Chinese vaccines and 4.5 million doses of Pfizer-BioNTech. Russia has also shared the patent and production of Sputnik V in Brazil, India and South Korea.
After Lancet magazine published its article on about Sputnik V reaching a 91.6% success rate in end-stage trials with 20,000 participants, it seems that more countries will follow Hungary to approve and use Sputnik V instead of waiting for Western pharmaceutical giants.
Benefits for people
 |
|
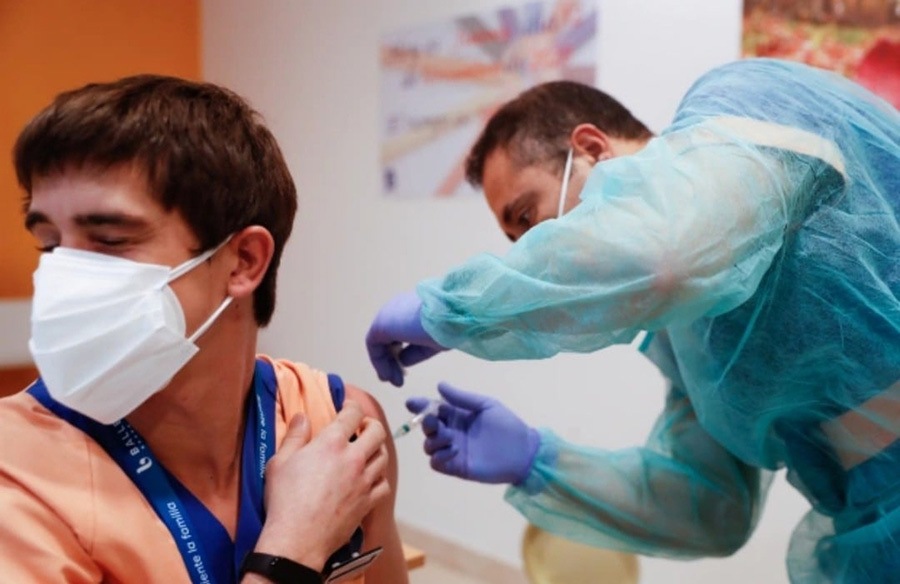
A healthcare worker in Madrid (Spain) is vaccinated against Covid-19. Photo: Reuters
|
Promoting the share of vaccine patents and technologies is therefore a political boon for Western nations.
On the other hand, some scientists believe that the new vaccines developed by Moderna, Pfizer-BioNTech and an under-developed mRNA vaccine are easier to produce, and easy to expand production scale. With technology transfer, new production capacity, including an mRNA vaccine, this could increase in a few months.
A year ago, there was no company in the world that produced the mRNA vaccine on a large scale. Now hundreds of millions of doses are being produced. Many vaccine producers have built dozens of factories - most of them set up in less than six months. For example, the Swiss company Lonza planned to produce the Moderna vaccine in two months after receiving know-how.
Such rapid progress can be reached by low- and middle-income countries. For example, Biovac and Aspen in South Africa, Pasteur Institute in Senegal, Vacsera in Egypt, Serum Institute of India, etc. can rapidly restructure factories to produce mRNA vaccines. And there are many other opportunities around the world.
The financial problem is not a challenge either. The World Bank spent $12 billion to finance the development and access to vaccines, announced last October, as part of the overall package of up to $160 billion of the World Bank Group to June 2021. This aimed to help developing countries fight the Covid-19 pandemic. At least $4 billion through the IFC for vaccine production has, in fact, been negligible, due to the lack of efforts to transfer know-how and technology.
Opening up vaccine technology and helping countries around the world, especially developing countries, could help end the pandemic on a global scale. For developing countries, in addition to efforts to purchase and develop vaccines, there should also be a readiness to organize production when they are shared, and beyond that, initiatives should be promoted to help the produce vaccines soon for themselves and the community.
Pham Quang Vinh
Vaccine nationalism
Vaccine nationalism has become alarming, as politicians have criticized the previous US President Donald Trump for his "America First" doctrine.